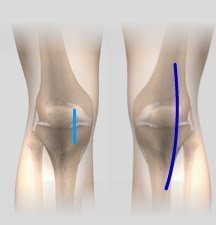
Minimally Invasive Knee Joint Replacement
Total knee replacement is a very successful surgical treatment for knee arthritis. Over the years, minimally invasive knee replacement surgical techniques have been developed to lessen tissue trauma and improve patient outcomes. This minimally invasive approach involves much smaller incisions than the usual 10-12 inch incisions used in the traditional knee replacement and spares the quadriceps muscle and tendon, which control bending of the knee, from being cut to access the knee joint.
The smaller incisions with minimally invasive surgery mean fewer tissues are cut resulting in quicker healing and recovery. The potential advantages of minimally invasive joint replacement surgery are:
- Minimal surgical dissection
- Shorter recovery period
- Shorter hospital stay
- Reduced post-operative pain
Procedure
Minimally invasive surgery for knee replacement involves the use of smaller incisions which are only 4 to 6 inches in length as compared to the 10-12 inch long incision used in the traditional procedure.
- Surgery is performed under sterile conditions in the operating room under spinal or general anesthesia. You will be lying on your back on the operating table with a tourniquet applied to your upper thigh to reduce blood loss.
- Your surgeon will then make an incision along the affected knee to expose the knee joint. The surgeon first focuses on the femur (thighbone). The damaged portions of the femur are cut at the appropriate angles using specialized tools.
- Then the femoral component is attached to the end of the femur with or without bone cement. The next step involves removal of the damaged area of the tibia (shinbone) and the cartilage. It allows for a smooth surface to which implants can be attached.
- The tibial component is then secured to the end of the bone using bone cement or screws. Your surgeon will place a plastic piece called an articular surface between these implants to ensure a smooth gliding movement.
- This plastic insert acts in a similar way as the original articular cartilage and helps in supporting your body weight as well as allows the femur bone to move over the tibia. The femur and the tibia bone with their new components are put together to form the new knee joint.
- To ensure that the patella (knee cap) glides smoothly over the new artificial knee, its rear surface is prepared to receive a plastic component. With all its new components in place, the knee joint is examined through its range of motion.
- All excess cement will be removed and the entire joint will be irrigated or cleaned out with a sterile saline solution.
- The incision is then closed and drains are usually inserted. A surgical dressing or bandage is then placed over the incision.
As there is less tissue damage around the knee during the minimally invasive procedure surgery, you can expect a shorter hospital stay, faster recovery and also avoid an unsightly smaller surgical scar.
