Unicompartmental/Partial Knee Replacement Surgeon in Santa Monica, Encino, CA

Older people with osteoarthritis that is confined to a single compartment of the knee are candidates for unicompartmental knee replacement, in which only the damaged compartment of the knee is replaced with an implant. Erik N. Zeegen, M.D. provides diagnosis and minimally invasive unicompartmental knee replacement in Santa Monica,Encino & Thousand Oaks. Erik N. Zeegen, M.D. also provides the highest level of care during and after the surgery. Contact Erik N. Zeegen, M.D.'s office for an appointment today!
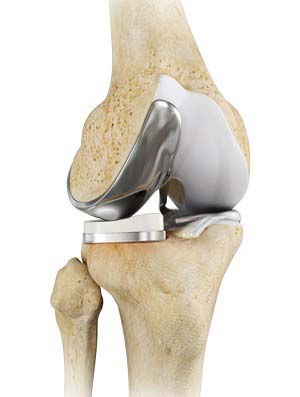
What is Unicompartmental Knee Replacement?
Unicompartmental knee replacement is a minimally invasive surgery in which only the damaged compartment of the knee is replaced with an implant. It is also called a partial knee replacement.
The knee can be divided into three compartments: patellofemoral, the compartment in front of the knee between the kneecap and thighbone, the medial compartment, on the inside portion of the knee, and lateral compartment which is the area on the outside portion of the knee joint.
Disease Overview of Arthritis
Arthritis is the inflammation of a joint that causes pain, swelling (inflammation) and stiffness.
Osteoarthritis is the most common form of knee arthritis, in which the joint cartilage gradually wears away. It most often affects older people. In a normal joint, articular cartilage allows for smooth movement within the joint, whereas in an arthritic knee the cartilage itself becomes thinner or completely absent. In addition, the bones become thicker around the edges of the joint and may form bony spurs. These factors can cause pain and restricted range of motion in the joint.
Diagnosis of Arthritis
Your doctor will diagnose osteoarthritis based on your medical history, physical examination, and X-rays. X-rays typically show a narrowing of joint space in the arthritic knee.
Treatment for Arthritis
There are many treatments indicated for arthritis – both conservative and surgical. Your doctor will discuss the best option depending on your individual condition.
Indications of Unicompartmental Knee Replacement
Traditionally, total knee replacement was commonly indicated for severe osteoarthritis of the knee. In total knee replacement, all worn out or damaged surfaces of the knee joint are removed and replaced with new artificial parts. Partial knee replacement is a surgical option if your arthritis is confined to a single compartment of your knee.
Your doctor may also recommend surgery if non-surgical treatment options such as medications, injections, and physical therapy have failed to relieve the symptoms.
Surgical Procedure of Unicompartmental Knee Replacement
During the surgery, a small incision is made over the knee to expose the knee joint. Your surgeon will remove only the damaged part of the meniscus and place the implant into the bone by slightly shaping the shinbone and the thighbone. The plastic component is placed into the newly prepared area and secured with bone cement. Now, the damaged region of the femur or thighbone is removed to accommodate the new metal component, which is fixed in place using bone cement. Once the femoral and tibial components are fixed in proper place the knee is taken through a range of movements. The muscles and tendons are then repaired and the incision is closed.
Postoperative Care Following Unicompartmental Knee Replacement
You may walk with the help of a walker or cane for the first 1-2 weeks after surgery. A physical therapist will introduce you to an exercise program to follow for 4 to 6 months to help maintain range of motion and restore your strength. You may perform exercises such as walking, swimming, and biking but high impact activities such as jogging should be avoided.
Risks and Complications Following Surgery for Unicompartmental Knee Replacement
The possible risks and complications associated with unicompartmental knee replacement include:
- Knee stiffness
- Infection
- Blood clots (Deep vein thrombosis)
- Nerve and blood vessel damage
- Ligament injuries
- Patella (kneecap) dislocation
- Wearing of the plastic liner
- Loosening of the implant
Advantages of Unicompartmental Knee Replacement
The advantages of unicompartmental knee replacement over total knee replacement include:
- Smaller incision
- Less blood loss
- Quick recovery
- Less postoperative pain
- Better overall range of motion
- Feels more like a natural knee
If you would like to have additional information on the treatment of various knee conditions or would like to learn more about unicompartmental/partial knee replacement, please contact Erik N. Zeegen, M.D., serving the communities of Santa Monica, Encino, CA.
